Medical Team
| Name |
Specialties |
|
Shih-Yi Lin
|
Internal Medicine, Diabetes, Endocrinology, Thyroid, Geriatrics |
|
Yu-Shan Lee |
Cerebrovascular disease, dizziness, dementia, geriatrics |
Shuo-Chun Weng |
Internal Medicine Gerontology (falls, integration of polypharmacy, senile syndrome,chronic kidney disease in the elderly) Nephrology (glomerulonephritis, hemodialysis, peritoneal dialysis) |
|
Yin-Yi Chou |
Geriatric rheumatology, general immune rheumatology, degenerative arthritis,
osteoporosis, allergies for the elderly |
|
Fu-Hsuan Kuo |
Cerebral stroke, headache, dizziness, unsteady gait, tremor, slow movement and other geriatric syndromes in geriatric medicine (gait imbalance/easy to fall,weakness, dementia, delirium, malnutrition, etc.), integrated care (elderly chronic disease comorbidity and polypharmacy tidy) |
|
Cheng-Fu Lin |
Family Medicine, Occupational Medicine, Geriatrics, Hospice, Preventive Medicine,Obesity Medicine |
Organizations
There are 6 attending physicians (including the director), 1 fellow, 17 clinical geriatric educator, 5 administrative, and 1 clinical research assistants. We divide our team into several task groups in charge of: geriatric clinical health care in wards and the outpatient clinic, post-acute care, intermediate-, long-term, veterans home and community care, and research and education training, to provide a comprehensive care for older people in central Taiwan. For clinical services in the hospital, there are a 10-bed geriatric acute care unit, and 10 weekly integrated geriatric outpatient clinics.

Clinics
In the outpatient clinic, we provide diagnosis of, and treatment for, common diseases in the elderly as a whole, through physical, psychological, social and functional assessment. Rather than a conventional “organ-specific” medical approach, we focus upon commonly seen geriatric symptoms (e.g: falls, dementia, depression, dizziness, insomnia, urinary incontinence, constipation, frailty, polypharmacy, nutrition problems, and disability), aiming at functional optimization and restoration. By utilizing the joint specialties service in the one-stop clinic, the patients and their family can eliminate unnecessary trips from home to the hospital. Through comprehensive geriatric assessments and care, the geriatric syndrome can be highlighted and hence we can make individualized care plans for each senior patient.

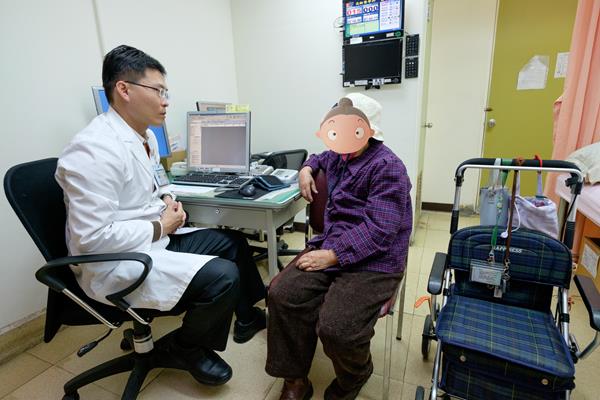
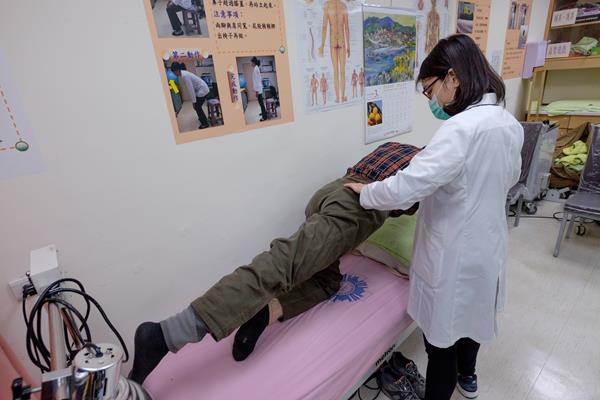
Wards
In the geriatric acute care ward, we generally take care of elderly patients with acute illness, multiple medical problems and common geriatric syndromes (e.g. delirium, falls, incontinence, dementia, malnutrition, and immobilization) and disabilities, in a safe and supportive environment. In addition, we provide multidisciplinary medical services according to the individual needs of the elderly, and the medical team members include physicians, nurses, social workers, physiotherapists, occupational therapists, language therapists, dietitians, and pharmacists, who focus on human considerations.


Post-acute care
In accordance with the Taiwan NHI program for post-acute care (PAC) plan for stroke, we have a medical service for transferring acute stroke patients in the hospital, to sub-acute rehabilitation or long-term care facilities to improve patient outcome and reduce costs. In the cooperation hospitals, physical, occupational, and speech therapy are continuously provided.

Consultation
In the hospital, we provide recommendations for the comprehensive management of older patients, including pre- and post-op assessments, assistance in transferring to long-term care, management of geriatric syndromes, home-based care, and psychosocial support. Through the process of consultation, the geriatricians communicate with medical staff in other departments to improve care quality in hospitalized elderly.

Intermediate- and long-term care in community and local Veterans hospital
To address continuous care coordination between acute and Intermediate- and long-term care services, we consult and refer inpatients who still need local hospital or institutional or nursing home care after discharge. The enrollees include the physically and psychologically disabled, those with high daily activity dependence, those who lack family care resources, or those who cannot be cared for in the community and at home, and need technical nursing care services (e.g. foley catheters, nasogastric tube and trachea tube replacement, and wound dressing). In the community, our doctors or nurses provide home visits to bed-ridden or mobility disabled patients, to assess the problems encountered by the elderly.

Geriatric medicine specialty training and education and research
A 1-year training program with curricula in the fields of geriatric medicine core knowledge, inpatient geriatric care, community-based geriatric medicine, elderly long-term care, geriatric palliative medicine, geriatric rehabilitation and geriatric neurology is provided in the hospital. The aim is that trainees will become qualified in geriatric medicine through training designed to include ward care, clinic service, lectures, presentations and educational courses. In addition, research and publication training will be instructed by the senior geriatric medicine teachers, and we have a regular academic meeting with other hospitals in central Taiwan. Also, we cooperate with Tung-Hai University, and Changhua and Taichung-Changhua Veterans homes to form an integrative group to improve geriatric research and training for geriatric care personnel.

